Understanding And Living With Lipedema
Lipedema is a long-term chronic health issue that affects millions of people worldwide. Characterized by the abnormal buildup of body fat, mainly on the lower part of the body, lipedema remains widely misunderstood and often misdiagnosed.
In this article we will review the following topical areas concerning lipedema:
- What Is Lipedema
- What Causes Lipedema / Lipedema Causes
- How Common Is Lipedema
- What Are Risk Factors For Getting Lipedema
- Identifying Lipedema Symptoms / Signs Of Lipedema
- What Are The Types Of Lipedema
- Stages Of Lipedema
- What Are The Complications Of Having Lipedema
- How Is Lipedema Diagnosed
- What Is The Treatment For Lipedema / Lipedema Treatment
- How Can The Risk Of Getting Lipedema Be Lowered
- Living With Lipedema
What Is Lipedema
Lipedema is a long-term health condition which mainly affects women and causes abnormal fat buildup in the lower part of your body. This lipedema fat most often involves the butt, thighs and calves and gets worse over time. People with lipedema may see the condition develop in their hips or upper arms (lipedema in arms), however lipedema doesn’t develop in or affect the hands or feet. What is lipedema fat? Unlike most fat accumulation patterns, lipedema fat develops symmetrically, meaning that it affects both sides of the body equally, differentiating it from conditions like lymphedema, which often affects only one limb.
Oftentimes lipedema is confused with being overweight or having lymphedema, but lipedema is a completely different condition involving the abnormal distribution of fatty tissues within the body. Lipedema vs lymphedema - while lipedema is not primarily a lymphatic disorder, it can eventually impact lymphatic function as the condition progresses leading to the development of lymphedema. Lipedema fat doesn’t respond to diet and exercise like ordinary body fat typically does. Having lipedema can cause pain and swelling resulting in tender skin that easily bruises. Lipedema can also result in lipedema fibrosis, which is the development of hardened scar tissue that occurs with the buildup of fat tissues, and is characterized by hard lipedema nodules underneath the skin which can be felt by gently pressing on the affected limb.
Living with lipedema can make normal daily activities difficult to perform and can negatively impact your overall quality of life. Although there isn’t a cure for lipedema, treatment for lipedema can help you feel better and make it easier to live a normal, active lifestyle. Early recognition and diagnosis of lipedema symptoms, along with an appropriate treatment protocol can help you manage the symptoms and slow the progression of the condition.
Lipedema Causes
Scientific evidence has not led us to understand if there is an exact cause of lipedema, or what causes lipedema in general. Instead, research has suggested that a combination of factors likely contributes to its development. Since most observed cases of lipedema have a family connection, genetic predisposition appears to be a significant factor of lipedema being passed from parents to their children. Lipedema runs almost exclusively in women, leading researchers to believe that it may have a connection to hormones. The signs of lipedema often begin to appear during hormonal shifts such as puberty, pregnancy, or menopause. While being obese doesn’t directly lead to or cause lipedema, more than half the people with it have a BMI greater than 35.
How Common Is Lipedema
Research has estimated that 1 in 72,000 people have lipedema. However, since lipedema is frequently misdiagnosed as simply being obese, the actual rate of occurrence is likely much higher. Lipedema in males is rare, with most diagnosed conditions being observed in women.
Risk Factors For Getting Lipedema
The following are factors that indicate a higher risk of developing lipedema:
- being female
- having a family history of lipedema
- having a BMI higher than 35
Lipedema Symptoms And The Signs Of Lipedema
Do I have lipedema? The most common and obvious signs of having lipedema include:
- an even buildup of fat (lipedema fat) on both sides of the buttocks, hips, thighs, calves or upper arms
- fat that does not go away with diet or exercise
- mild to severe pain
- heavy feeling in the legs
- swelling
- fibrotic bumps inside the fat (feels like there is something under the skin)
- skin that bruises easily
- excess fatigue (feeling more tired than usual)
- in later stages of lipedema, the development of lymphedema
Types Of Lipedema
There are five different types of lipedema that you may experience, with each type being used to describe the location of excess fat (lipedema fat) within the body. A person can have more than one type of lipedema, as determined by the location of the excess fat or lipedema fat.
The types of lipedema and related locations of excess lipedema fat include:
- Type I lipedema: buttocks
- Type II lipedema: lipedema legs - buttocks, hips, and thighs
- Type III lipedema: lipedema legs - buttocks, hips, thighs and calves
- Type IV lipedema: lipedema arms
- Type V lipedema: lipedema legs - calves (knees to ankle)
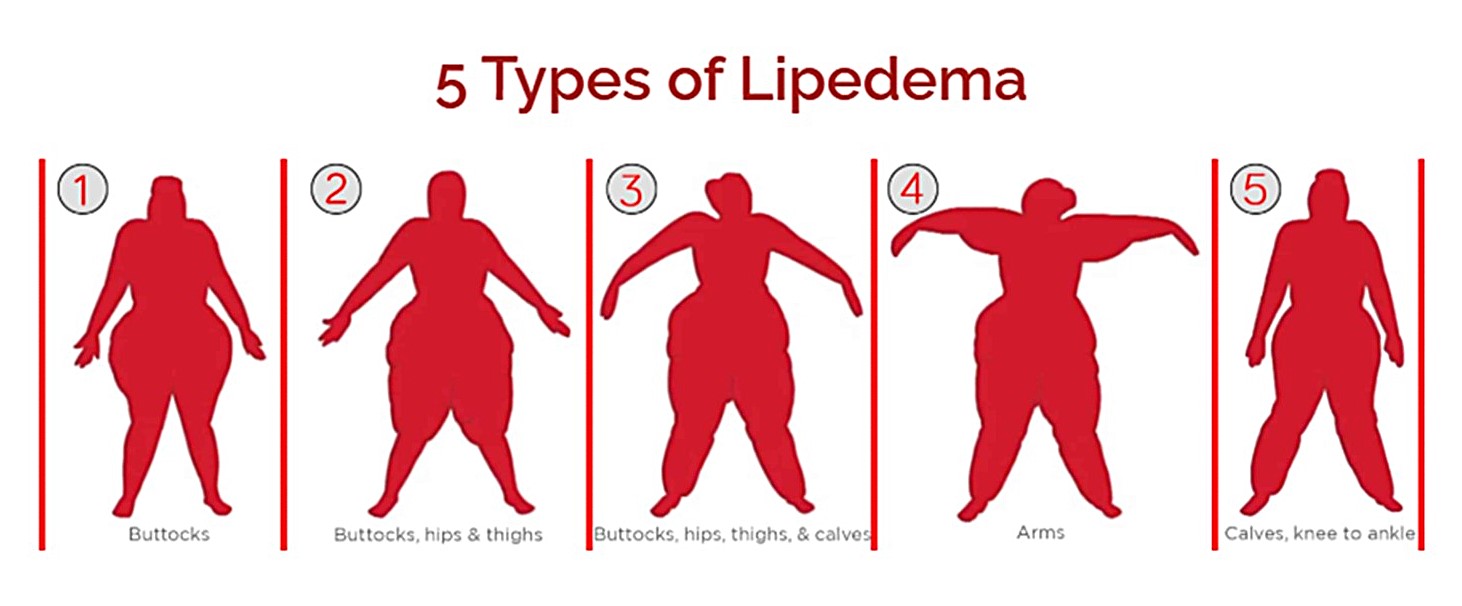
Courtesy of The Lipedema Project
Stages Of Lipedema / Lipedema Stages
Once it develops, lipedema generally will slowly worsen with time. The development of lipedema has be categorized within one of four progressively worse stages of lipedema. These four stages of lipedema are as follows:
Stage 1 Lipedema: In the earliest and mildest form of lipedema (lipedema stage 1), the skin looks normal, but small nodules (feel like pebbles) develop within fatty deposits under your skin. Mild tenderness, discomfort or pain and bruising can appear with stage 1 lipedema. While the lymphatic system will generally continue to function adequately, you may begin to experience minor fluid retention alongside the fatty deposits. Normally lipedema can be treated with compression (compression stocking for lipedema), diet and exercise at this stage.
Stage 2 Lipedema: As the fatty tissue builds up (lipedema fat), the texture of the skin surface changes to having an uneven or “dimpled” appearance similar to but more pronounced than cellulite, and the underlying nodules grow larger in both size and number. Pain levels increase with more widespread tenderness, along with constant aching or heaviness in the limbs and increased fatigue. Since lipedema generally does not affect the feet, with lipedema in legs the appearance of an “ankle cuff” will develop as the fatty tissue within the calves begins to accumulate. At this stage, the symptoms of lipedema also begin to extend beyond just the physical appearance and begin to affect mobility and comfort. With stage 2 lipedema treatment becomes increasingly more important, requiring more rigorous compression and lymphatic massage to prevent progression to stage 3 lipedema, where irreversible tissue changes begin to occur.
Stage 3 Lipedema: This is the advanced stage of lipedema, which is characterized by fatty tissue volumes that have significantly increased and increasingly become hardened and firm, referred to as lipedema fibrosis. Significant distortion of the fatty tissue begins to develop, along with large overhanging folds or lobes of skin and fatty tissue, particularly around the knees and thighs. The fatty tissue on legs may begin to stick out, making it hard to find properly fitting clothes, to walk and negatively impacts overall mobility. Severe bruising can occur from even minor contact, while the affected tissues become extremely painful and tender. During this stage, the lymphatic system oftentimes becomes compromised, leading to the accumulation of fluid within the tissues. On top of the physical symptoms, stage 3 lipedema oftentimes leads to significant emotional distress, which manifests in depression, anxiety and social isolation. Treatment at this stage will likely be more aggressive to help manage the symptoms and slow progression. The effects of having stage 3 lipedema cannot be reversed, but proper treatment will help reduce the discomfort and improve quality of life. In addition to pain medications and anti-inflammatories, complete decongestive therapy combined with layered compression probably will be introduced. Treating stage 3 lipedema will often require surgical treatment (lipedema surgery) such as liposuction and skin reduction surgery.
Stage 4 Lipedema: The final advanced stage of lipedema development is referred to as lipo-lymphedema, which means that you have both lipedema and lymphedema at the same time. With lipo-lymphedema there exists both lymphatic blockage as well as excessive fatty tissue accumulation. Lipo-lymphedema requires specialized combined therapy for treating both lipedema as well as lymphedema, such as manual lymphatic drainage (MLD), complete decongestive therapy (CDT), and wearing medical grade compression wraps.
Complications Of Having Lipedema
Having lipedema can impact your overall quality of life and lead to:
- difficulty with walking
- venous (vein) disease
- flat feet
- joint issues
- knock knees (knees touch each other when your feet are apart)
- secondary lymphedema or lipo-lymphedema (blockage in the lymphatic pathway resulting in lymph fluid to build up)
- infection (cellulitis)
- feelings of embarrassment and anxiety
- depression
Diagnosing Lipedema / Do I Have Lipedema
Early diagnosis allows for earlier intervention and treatment of lipedema. Unfortunately, lipedema is often misdiagnosed as obesity, as lymphedema or simply dismissed as having experienced weight gain. While a person who suffers from lipedema may also be obese, the two conditions (lipedema and obesity) are not directly related to one another. What is lipedema fat? The painful nodules contained within fatty deposits (lipedema fat) make lipedema different from ordinary body fat. Also, with lipedema in legs there is a clear difference in size between the affected lipedema legs and unaffected feet (or arms and hands). Lipedema vs cellulite - lipedema is also often confused with cellulite which is a common skin condition characterized by lumpy, dimpled skin caused by fat deposits within the skin.
Lipedema can usually be diagnosed during a physical exam and based on your individual and family medical histories. Your healthcare provider may also want to do tests to rule out other health conditions, such as cellulitis, lymphedema or circulatory issues such as chronic venous insufficiency.
Lipedema Treatment / How To Treat Lipedema
If you have lipedema, you may ask how to get rid of lipedema? While currently there is no cure for lipedema, there are a variety of lipedema treatment methods that can be prescribed for helping manage lipedema symptoms, reducing pain and inflammation, and slowing the condition's progression. The treatment for lipedema includes protocols which will typically be tailored to each person’s lipedema symptoms and stages of lipedema.
Noninvasive lipedema treatment
How to treat lipedema? Simple treatment for lipedema may include the following:
- Exercise: simple low-impact exercises such as swimming, biking and walking can help with weight management, promote circulation, improve mobility and reduce swelling. Exercising in a pool can help reduce stress on the joints.
- Heart-healthy, low-carb, anti-inflammatory lipedema diet: while this won’t affect the underlying fatty tissue, a healthy lipedema diet may help slow the progression of lipedema.
- Skin care: keeping your skin clean and moisturized will help maintain overall skin health around the affected areas to help prevent infection such as cellulitis.
- Medications or supplements: your healthcare provider may prescribe certain medications to help with inflammation, swelling and pain.
Depending on the stage of the lipedema, other noninvasive treatment for lipedema may be prescribed, including:
- Compression therapy: compression, such as wearing a compression wrap or compression stocking for lipedema in legs, compression sleeves for lipedema in arms, leggings or compression shorts can help with swelling (edema) and promote circulation.
- Manual Lymphatic Drainage (MLD): this is a specialized, gentle massage technique that stimulates lymph fluid and helps reduce edema (swelling) in lipedema legs.
- Complete Decongestive Therapy (CDT): this combines both the manual lymphatic drainage (MLD) massage followed by wearing a compression bandages or a garment (usually a compression wrap) to help maintain the volume reduction in lipedema legs obtained by the MLD.
- Pneumatic Compression Device: a compression pump is a mechanical means for providing pressure to your lipedema legs to help reduce swelling and promote fluid flow and lymphatic drainage.
Invasive lipedema treatment
In the more extreme lipedema stages invasive surgical treatment (lipedema surgery) may be necessary to help alleviate pain and swelling. Invasive treatments / types of lipedema surgery include the following:
- Liposuction: this is used to remove fatty tissue, help reduce pain and improve mobility.
- Bariatric surgery: when lipedema exists with a BMI exceeding 35, your healthcare provider may recommend bariatric surgery to help manage and control your weight.
- Excision surgery: may be used for advanced stages of lipedema to remove large, fibrotic, or nodular tissue deposits.
- Skin Removal Surgery: After fat removal or loss, a skin removal procedure may be necessary for sagging skin.
Lowering The Risk For Lipedema
Since we do not know exactly what causes of lipedema or lipedema causes, it makes it difficult to avoid getting it. However, if you have some of the risk factors for developing lipedema (being female and/or having a family history of lipedema), the best prevention against getting lipedema that you can control is to maintain a healthy weight, through proper diet and exercise.
Living With Lipedema
While some people with lipedema will have mild symptoms that don’t get worse with time, many have lipedema that progressively worsens with time. Regardless of the type and severity of lipedema, early diagnosis and treatment for lipedema is the best solution should it develop It will be very important to follow the lipedema treatment plan that your healthcare provider prescribes. Exercise, weight loss and compression will help lead to a better lipedema treatment outcome, while medications and surgical intervention can help you feel better. Counseling or support groups can help provide the mental and emotional support that you need to help navigate the psychological impact of living with lipedema.

